Scientists identify key role of divisive Alzheimer’s protein
pharmafile | February 8, 2017 | News story | Research and Development | Alzheimer's
Researchers from the Stark Neurosciences Research Institute at Indiana University have claimed to have finally identified the purpose of an immune system protein that has divided scientists on its function within patients suffering from Alzheimer’s, allowing for the development of an updated model of the disease.
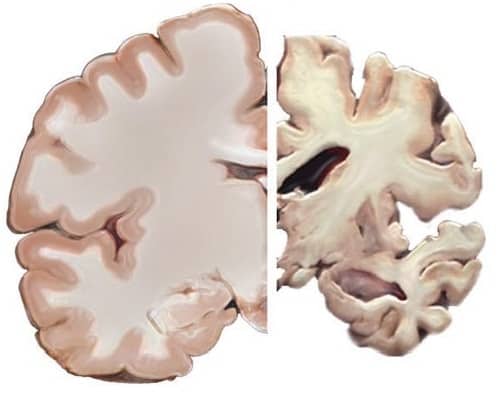
It has been determined that triggering receptor expressed on myeloid cells 2 (TREM2) works to help identify changes in the brain’s environment; as a response to the build-up of toxic amyloid protein plaques associated with Alzheimer’s, the receptor gathers immune cells as a defence mechanism.
However, a surge of these cells can also cause negative effects alongside positive ones, which has had researchers at odds, as notes Taylor Jay, lead study author and graduate student in the department of neurosciences at Case Western Reserve University School of Medicine:
“Our lab and others had previously published conflicting results about how TREM2 affected pathology in Alzheimer’s mouse models,” she explained. “One group published data showing Alzheimer’s mice lacking TREM2 had more amyloid plaques. We previously found the opposite, that getting rid of TREM2 improved amyloid pathology. We didn’t know why we weren’t getting the same answers. And, that was just the first question we wanted to ask, before we moved onto questions about exactly how TREM2 was influencing pathology.”
According to the study, the confusion arises due to TREM2’s varying functions both early and late in progression of the disease. In early stages, the removal of TREM2 helps to eliminate the toxic amyloid plaques in the brains of mice, but the reverse is true late in the disease – the plaques became enlarged in the absence of TREM2.
These findings may call for stage-specific models of the disease as well as subsequent approaches, and could have significant implications of the timing of patient treatments. Jay and her team now plan to corroborate their findings using other existing animal models of the disease.
“Our ultimate goal with these studies is to use an understanding of TREM2 function to understand the important roles that immune cells play in Alzheimer’s disease. Immune cells might not be all good or all bad throughout the course of Alzheimer’s disease progression,” she said.
Matt Fellows
Related Content

Lilly’s drug for early Alzheimer’s shows promising results
Eli Lilly (Lilly) has announced positive new data from the long-term extension of its phase …

Eli Lilly’s Kisunla approved by FDA for Alzheimer’s treatment
Eli Lilly has announced that the US Food and Drug Administration (FDA) has approved Kisunla …
FDA accepts Eisai’s Leqembi sBLA for early AD treatment
Eisai and Biogen have announced that the US Food and Drug Administration (FDA) has accepted …